When a vertebra in your spine collapses due to osteoporosis, trauma, or cancer, the pain can be unbearable. Standing, sitting, even breathing becomes a struggle. For many, traditional treatments like bed rest, painkillers, or braces offer little relief. That’s where kyphoplasty and vertebroplasty come in - two minimally invasive procedures designed to fix broken vertebrae and restore quality of life in hours, not months.
How These Procedures Work
Both kyphoplasty and vertebroplasty involve injecting medical-grade bone cement into a fractured spinal bone. The goal isn’t just to patch the crack - it’s to stabilize the bone, stop the pain, and let you get back on your feet. The process starts with a small needle inserted through your back, guided by real-time X-ray imaging. You’re awake but sedated, so you feel pressure but no pain. In vertebroplasty, the cement is injected directly into the fractured vertebra under pressure. It flows into the cracks and hardens in about 15 minutes, acting like internal scaffolding. The whole thing usually takes under an hour. Kyphoplasty adds a crucial step before the cement goes in. A tiny balloon is inserted into the fractured bone and gently inflated. This lifts the collapsed bone back toward its normal shape, creating a hollow space. Once the balloon is deflated and removed, the cement is carefully injected into that cavity. This extra step isn’t just for show - it can restore lost height in the spine and reduce the hunched posture that often follows a compression fracture.Which One Is Better? The Key Differences
It’s not about which procedure is "better," but which one fits your situation. If your fracture has caused a noticeable curve in your spine - a hunched back or loss of height - kyphoplasty is usually the go-to. Studies show it can restore 40-60% of the lost vertebral height. That’s not just cosmetic. Restoring height improves balance, reduces pressure on nearby nerves, and makes it easier to breathe and move. But if your fracture is stable and your spine hasn’t changed shape much, vertebroplasty works just as well. Both procedures give nearly identical pain relief. Patients report dropping from an average pain score of 8.2 out of 10 to 1.5 within 24 hours. That’s a game-changer for people who’ve been stuck in bed for weeks. The big difference lies in risk and cost. Vertebroplasty has a higher chance of cement leaking out of the bone - anywhere from 27% to 68% of cases. Most leaks don’t cause symptoms, but some can press on nerves or travel to the lungs. Kyphoplasty reduces that risk significantly, with leaks occurring in only 9-33% of cases. That’s why many doctors prefer it, especially for older patients with fragile bones. Cost-wise, kyphoplasty runs about 20-30% more than vertebroplasty. In the U.S., Medicare pays around $3,850 for kyphoplasty versus $2,950 for vertebroplasty. For many patients, that difference matters - especially if you’re paying out-of-pocket or have high deductibles.Who Gets These Procedures?
These aren’t for everyone. They’re meant for fractures that haven’t healed after 4-6 weeks of rest, pain meds, and bracing. If your fracture is old and healed, these procedures won’t help. The typical patient is over 65, often a woman. About 25% of women over 50 and 40% over 80 will suffer at least one osteoporotic vertebral fracture. That’s why these procedures are so common - over 100,000 are done in the U.S. each year. Doctors use MRI scans to confirm the fracture is fresh. You need to see bone marrow swelling on the scan - that’s the sign the fracture is still active and responsive to treatment. A simple X-ray isn’t enough.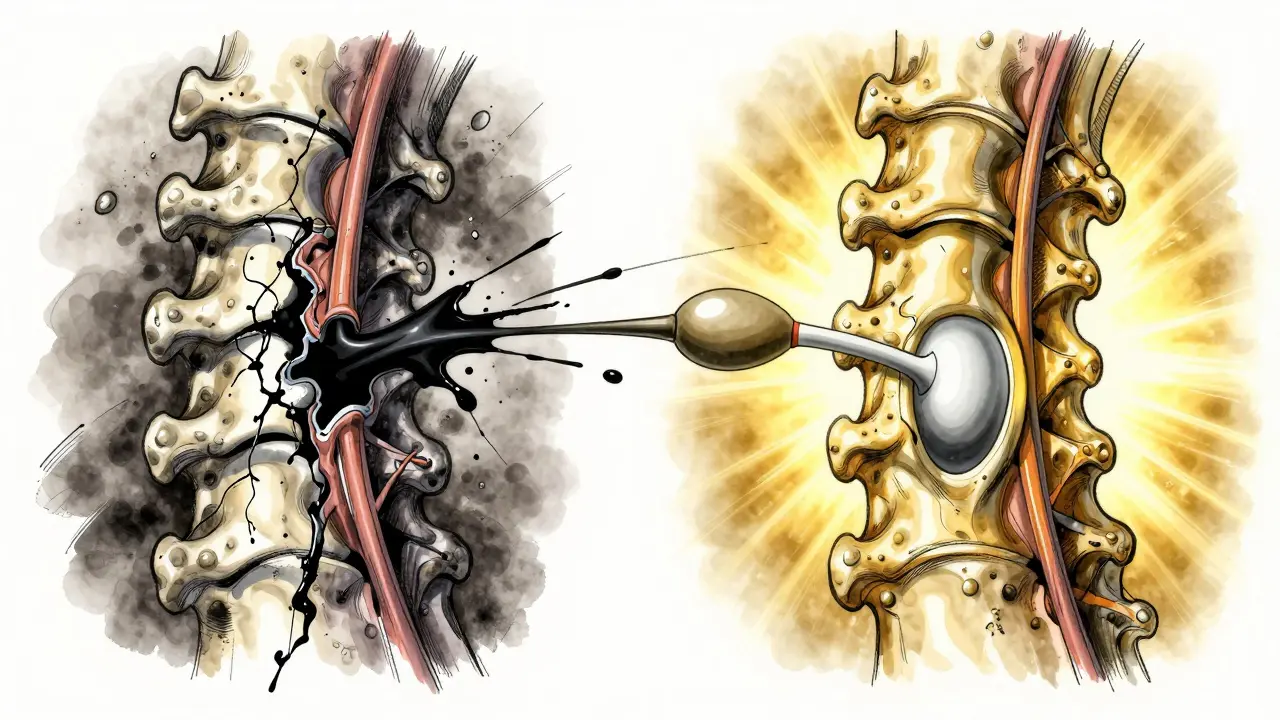
What to Expect After the Procedure
Most people go home the same day. You’ll need to lie flat for a few hours to let the cement harden completely. After that, you can start walking - slowly. You’ll be told not to lift anything heavy for a week, but light activities like walking and light housework are encouraged. Pain relief is often immediate. One patient on Reddit described it as "flipping a switch" - going from 9/10 pain to 2/10 within hours. Studies show 92% of patients return to normal daily activities within 72 hours. And 75% stop using opioid painkillers within a week. But it’s not magic. About 10-15% of patients still have some pain afterward. And in 5-10% of cases, another vertebra fractures within a year. That’s why treating the root cause - osteoporosis - is just as important as the procedure itself. Calcium, vitamin D, and bone-strengthening medications like bisphosphonates are usually started right after.What’s New in 2026?
The field is evolving. New types of bone cement, like calcium phosphate, are being used because they mimic natural bone better and generate less heat during hardening. In March 2023, Medtronic got FDA approval for an updated balloon system that’s easier to control and reduces procedure time. A major study published in The Lancet in January 2023 showed something surprising: getting treated within two weeks of the fracture lowered 12-month death rates by 28%. That’s huge. It suggests these aren’t just pain relievers - they might save lives by preventing complications like pneumonia or blood clots from long-term bed rest. The big question now is whether kyphoplasty’s height restoration actually leads to better long-term function. The COAST trial, ending in late 2024, is looking at whether patients who get their spine height restored truly walk better, stand taller, and avoid falls more than those who get vertebroplasty.
Real Talk: Pros and Cons
Kyphoplasty Pros:- Can restore spinal height and reduce kyphosis (hunchback)
- Lower risk of cement leakage
- Faster pain relief for severe deformities
- Preferred for fractures with significant collapse
- More expensive
- Longer procedure time
- Not always necessary if no deformity exists
- Lower cost
- Faster procedure
- Just as effective for pain relief
- Good for stable fractures without height loss
- Higher risk of cement leakage
- No height restoration
- Potential for worsening posture over time
What Experts Say
Dr. John Kallmes, who helped invent kyphoplasty, says the height restoration sounds impressive but doesn’t always translate to better daily function. "Both procedures relieve pain equally well," he notes. "The real value is in reducing complications, not just straightening the spine." Meanwhile, Dr. Richard Jensen’s cost analysis found vertebroplasty offers better value for healthcare systems - especially when deformity isn’t present. "We’re spending more for a benefit that doesn’t always show up in patient outcomes," he argues. The American Academy of Orthopaedic Surgeons gives both procedures a "moderate strength" recommendation. That means they’re proven to work, but the choice should be personalized.Final Thoughts
If you’re dealing with a recent vertebral fracture and pain isn’t improving, you have options. Kyphoplasty is ideal if you’ve lost height or have a visible curve in your spine. Vertebroplasty is a solid, affordable choice if your fracture is stable and your posture is mostly intact. The bottom line? Both work. Both are safe. Both let you walk out of the hospital the same day. The decision comes down to your fracture type, your goals, and your budget. Talk to your doctor, ask about your MRI results, and don’t be afraid to ask: "Which one makes the most sense for me?"Are kyphoplasty and vertebroplasty the same thing?
No. Both use bone cement to stabilize fractured vertebrae, but kyphoplasty includes a balloon step to restore height before injecting cement. Vertebroplasty injects cement directly without height restoration. Kyphoplasty is more complex and costly, but reduces cement leakage risk.
How long does recovery take after kyphoplasty or vertebroplasty?
Most patients go home the same day. You’ll need to rest for 24 hours and avoid heavy lifting for a week. Light walking and daily activities can resume within 72 hours. Full recovery, including returning to normal exercise, usually takes 1-2 weeks.
Do these procedures cure osteoporosis?
No. They treat the fracture, not the underlying bone weakness. After either procedure, you’ll need to start or continue osteoporosis treatment - calcium, vitamin D, and medications like bisphosphonates - to prevent future fractures.
Is kyphoplasty worth the extra cost?
It depends. If your fracture has caused noticeable spinal deformity or height loss, kyphoplasty’s ability to restore structure may improve posture and reduce future risks. If your fracture is stable with no deformity, vertebroplasty offers nearly identical pain relief at a lower cost.
Can these procedures be done more than once?
Yes. Many patients have multiple fractures over time, especially with ongoing osteoporosis. Each fracture can be treated separately, even in different areas of the spine. However, treating new fractures requires confirming they’re fresh (via MRI) and not old, healed injuries.


Bryan Woody
March 22, 2026 AT 04:21Chris Dwyer
March 23, 2026 AT 14:13Solomon Kindie
March 23, 2026 AT 19:01Natali Shevchenko
March 25, 2026 AT 11:14Nishan Basnet
March 27, 2026 AT 07:20Allison Priole
March 29, 2026 AT 08:06Casey Tenney
March 31, 2026 AT 04:54Sandy Wells
April 1, 2026 AT 12:35Timothy Olcott
April 1, 2026 AT 21:42